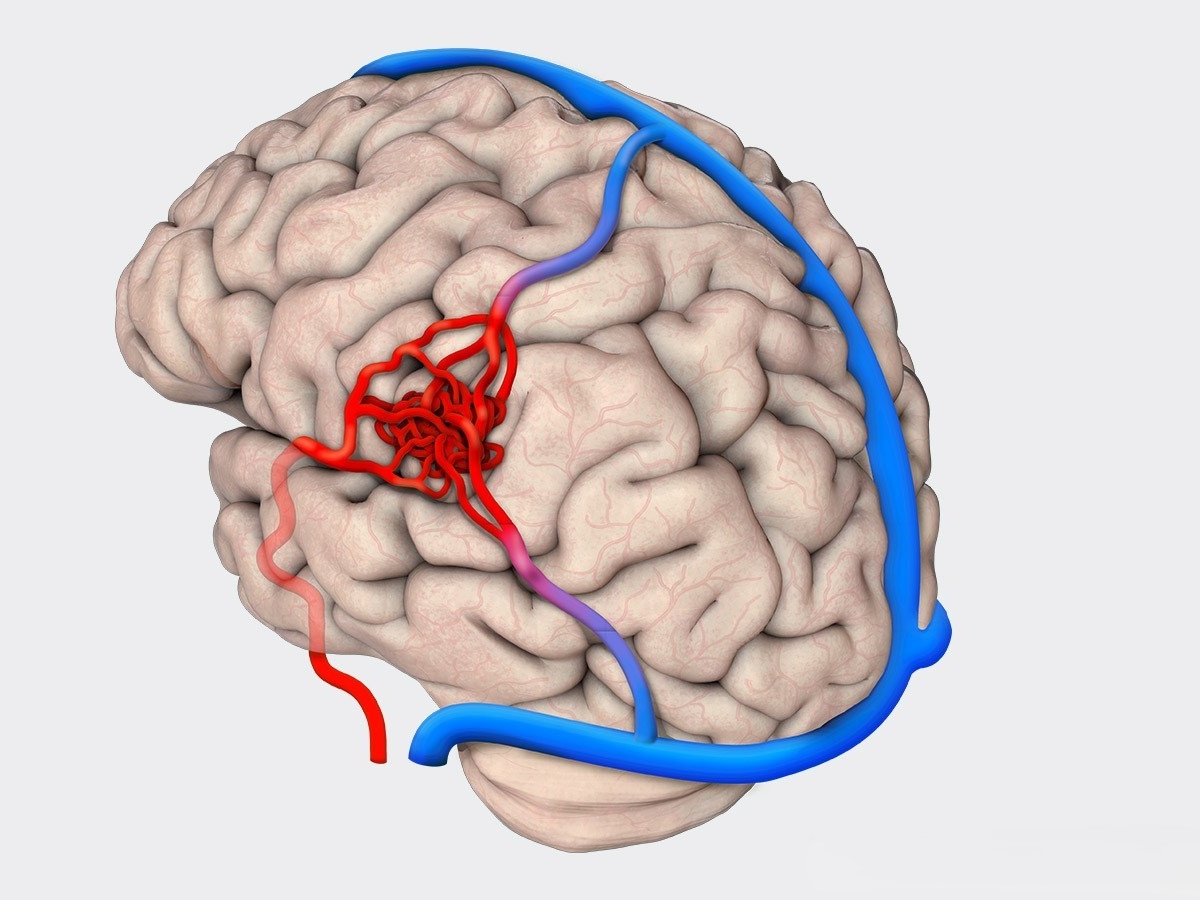
AVMs are evaluated with a combination of imaging studies:
AVMs are graded using the Spetzler-Martin scale (Grades I–V), which considers size, eloquence of adjacent brain, and pattern of venous drainage to estimate surgical risk. Dr. Choudhri is a contributor to the international MISTA Consortium, one of the world’s largest multicenter AVM research collaborations, with multiple publications analyzing treatment outcomes across all Spetzler-Martin grades.
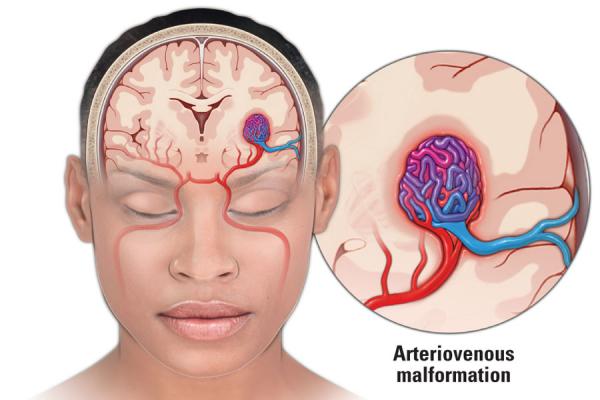

AVM treatment is often multimodal—meaning the best outcomes frequently come from combining two or more approaches. The treatment strategy is individualized based on the AVM’s grade, location, hemorrhage history, and patient factors.
Complete surgical removal of the AVM nidus is the definitive cure and remains the gold standard for low-to-moderate grade AVMs (Spetzler-Martin I–III). When successful, microsurgery provides immediate elimination of the hemorrhage risk. Dr. Choudhri employs advanced techniques including intraoperative angiography (performed through transradial access), neuronavigation, neurophysiological monitoring, and fluorescence guidance to ensure complete resection while preserving normal brain function.
Catheter-based delivery of liquid embolic agents (such as Onyx) into the AVM feeding arteries to reduce blood flow through the lesion. Embolization is most commonly used as a preoperative adjunct to surgery—shrinking the AVM and reducing its blood flow to make surgical resection safer—or to target specific high-risk features such as intranidal aneurysms.
Dr. Choudhri’s MISTA Consortium research includes landmark studies on the safety and efficacy of preoperative embolization in AVMs, including analysis of outcomes in AVMs with perinidal aneurysms and single draining veins.
Some AVMs—particularly those that are deep-seated, in critical brain regions, and have not hemorrhaged—may be most safely managed with careful observation and serial imaging. The decision not to treat is itself an active treatment decision that requires expert judgment.