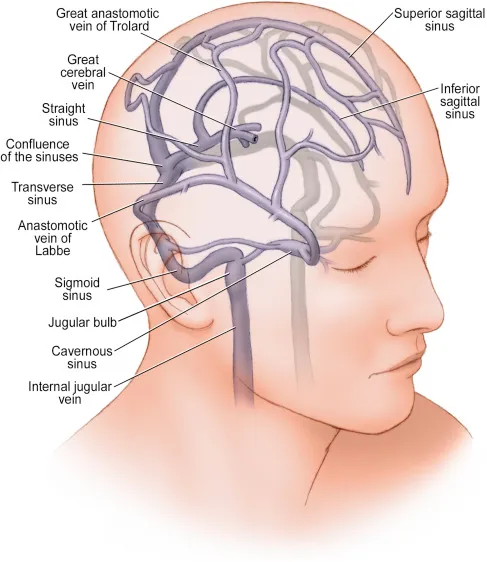
Narrowing of the major venous sinuses (most commonly the transverse and sigmoid sinuses) can impair drainage from the brain, leading to elevated intracranial pressure. Symptoms include headaches, pulsatile tinnitus, visual disturbances, and in severe cases, vision loss from papilledema. Venous sinus stenosis is frequently associated with idiopathic intracranial hypertension (IIH).
IIH is a condition of elevated pressure inside the skull without an identifiable structural cause. Patients experience severe headaches, pulsatile tinnitus, visual disturbances, and risk of permanent vision loss. IIH is increasingly understood to involve venous sinus stenosis as a contributing factor, and venous sinus stenting has emerged as an effective treatment option for selected patients.
Dr. Choudhri has published research on the role of stenting in venous sinus stenosis for IIH and is a contributor to the MPRESS trial, a PCORI-funded national study evaluating treatments for IIH. His team has also published on the emerging role of GLP-1 receptor agonists (such as semaglutide) in IIH management—an exciting new therapeutic avenue.
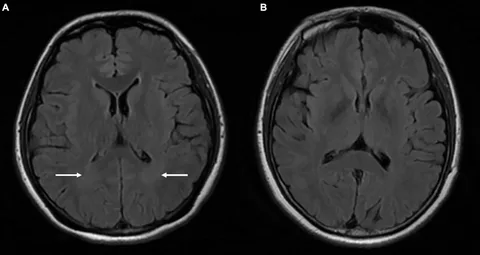

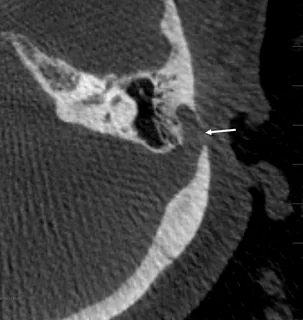
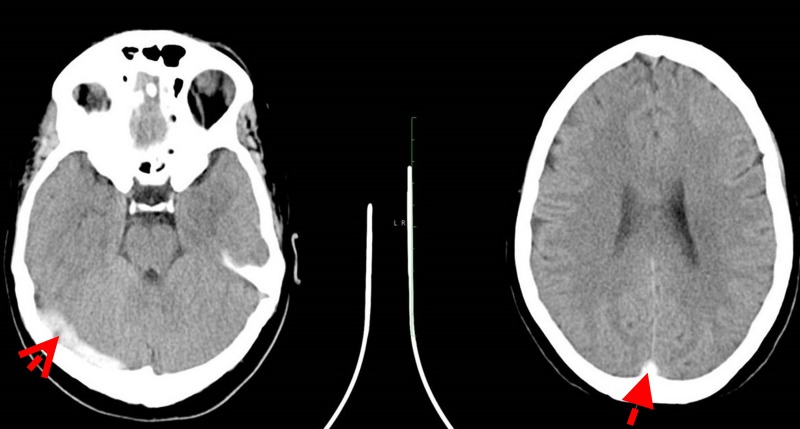
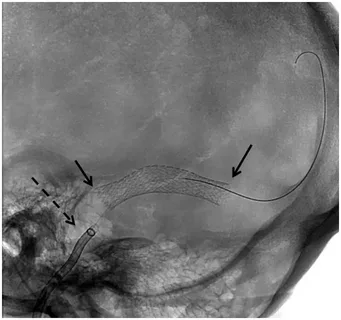
Dr. Choudhri’s team has published the largest single-center experience using upper extremity venous access for neurointerventional procedures. This approach allows venous interventions—including sinus stenting and venous diagnostic procedures—to be performed through the arm rather than the groin, improving patient comfort and reducing access-site complications.
The Choudhri Lab’s research in cerebral venous disease represents one of the most active and productive programs in the country, with publications spanning diagnostic innovation, treatment outcomes, and novel therapeutic targets. Dr. Choudhri was invited faculty at the SNIS Cerebral Venous and CSF Disorders Summit (2024, 2025) and the New York Venous Symposium (2025).
